Dental claims unpaid after a couple of weeks may not seem overdue. But consider this: you send most of your claims electronically, and hopefully you send your claims every single day. So, the claims arrive the same day. Insurance carriers typically process electronic claims within 14 days, which is why Dentrix Ascend defaults to 14 days to flag a claim and puts it into the Unresolved Claims area of your dashboard.
But not all carriers work at this level of efficiency, and a few claims may require some added attention from the insurance carrier. If 14 days seems like an unrealistic turnaround for a specific carrier, you can customize the expected period of insurance claim resolution and get a more exact picture of how many of your claims are overdue.
How to:
- Go to the carrier whose overdue claim timeframe you want to change. From within an overdue claim on the Unresolved Claims page, click Visit carrier page.
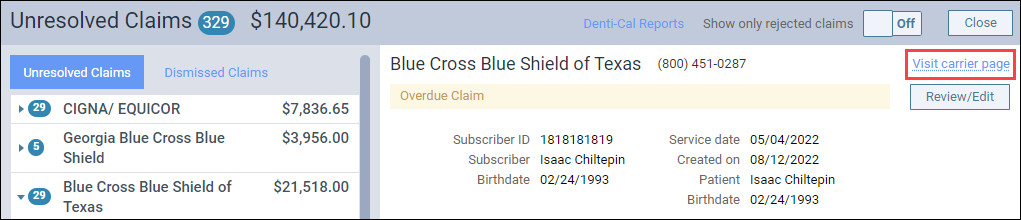
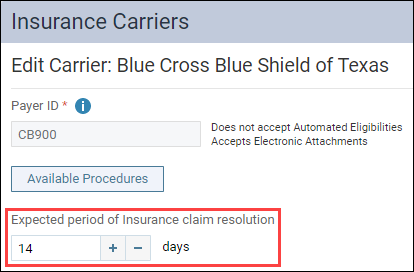
- In the Edit Carrier page, update the Expected period of Insurance claim resolution field to the number days to wait before Dentrix Ascend notifies you that claims from this carrier are overdue. Save your changes.
Additional Information
- There are other ways to get to the Edit Carrier page. You can use the Home menu, or you can click a link from a patient’s Insurance Information page.
- If you want to preemptively start making expected period changes, a good place to start configuring will be your carriers with Payer ID 06126, whose correspondence is by mail.
- Want to learn more about insurance carrier configuration? Watch the Adding an Insurance Carrier segment from the 5 Steps to Getting Patient Portion Estimates You Can Trust webinar in the Resource Center.

