How many times have you submitted a pre-determination or an insurance claim only to find that the insurance carrier requires additional attachments or documentation? It likely happens a lot. You may not realize it, but different carriers may require different types of attachments for the same procedure. Dentrix Ascend has automated attachment reminders that help you know exactly what each insurance carrier requires for specific procedures when you are submitting insurance pre-determinations and insurance claims. These reminders save you time and improve the revenue cycle of your practice because they help you avoid denied or delayed pre-determinations and claims.
Automated reminders appear on the following pages and/or dialog boxes:
- Claim Detail
- Pre-authorization Detail
- Patient Walkout
- Unsent Claims Report (from the Home menu)
- Unsent Claims (from the Overview page)
An orange warning icon ![]() appears to alert you when attachments are required by the patient’s insurance carrier. The exact appearance of the messaging varies depending on which page or dialog box you are in.
appears to alert you when attachments are required by the patient’s insurance carrier. The exact appearance of the messaging varies depending on which page or dialog box you are in.
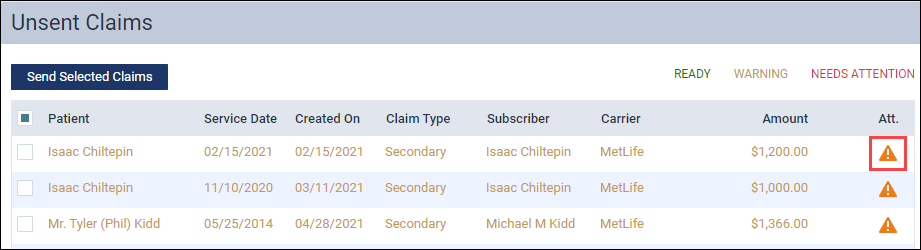
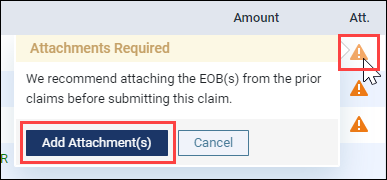
To view the attachment requirement, click the orange warning icon and then click Add Attachment(s) to open the claim or pre-determination.
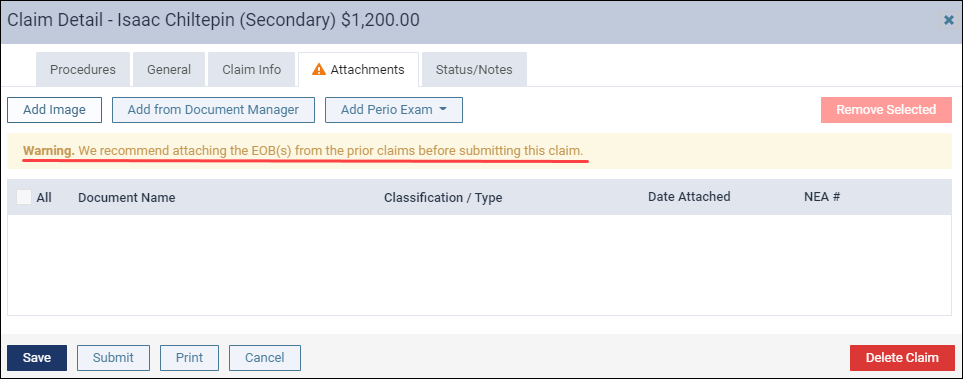
Note: A warning will also appear in the claim or pre-determination’s detail dialog box to alert you that attachments are required.
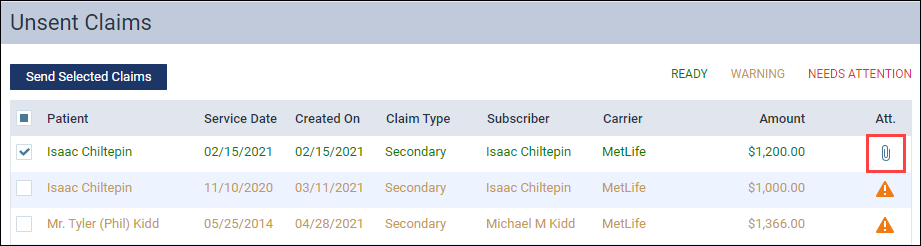
When you are finished adding the required attachments, the orange warning icon disappears and is replaced by the attachment icon.
Additional Information
- There is no option to turn off this warning notification feature.
- In cases where a secondary insurance claim needs an attachment, the warning message includes a recommendation to attach the EOB(s) from prior claims before submitting the claim.
- To learn more about how to add attachments to claims, watch Adding Attachments to Claims in the Resource Center.
