When multiple staff members enter patient information in Dentrix Ascend, there is a chance that duplicate insurance information can be entered. This often happens with insurance plans that have the same insurance carrier. The problem is that when there are two different versions of the same plan in Dentrix Ascend, coverage table information could be different between the two plans and estimates may not be calculated accurately for one plan.
Here are some general rules to follow when you are entering an insurance plan in Dentrix Ascend to avoid creating duplicates:
- Collect the patient’s insurance card, and make sure you have the insurance plan or employer’s name and the group number before you begin.
- Before you add a new plan, check to see if the plan already exists in Dentrix Ascend. First, find the carrier. Navigate to Home > Carriers. Search for the carrier by name or payer ID and select it.
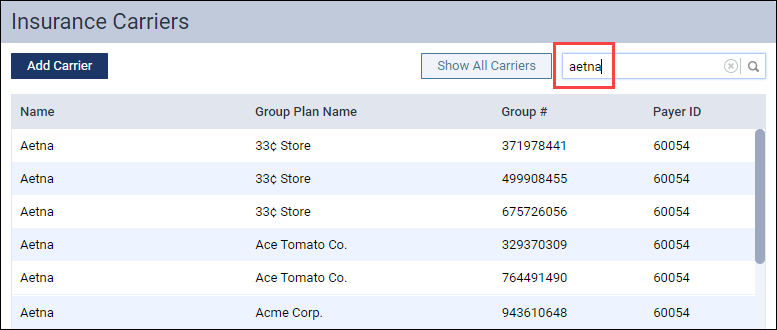
- Under Plans/Employers, search for the plan name or the group number to make sure that no plans exist. If the list is long, use the Search field to narrow down the choices. You can search by plan name or by group number.
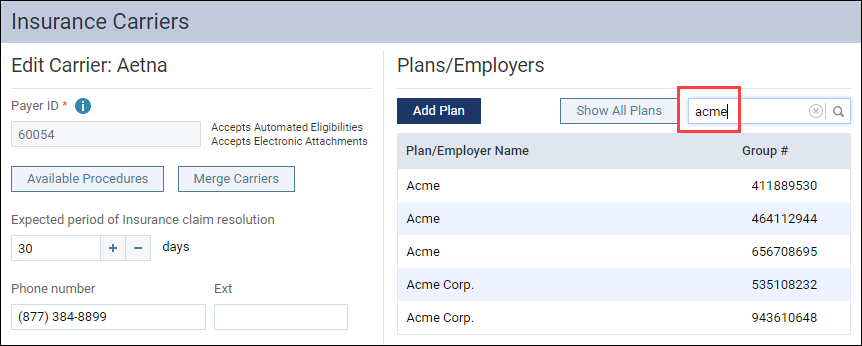
- Compare the group numbers to make certain your new insurance plan is not already in the system, because sometimes plan names can be similar.
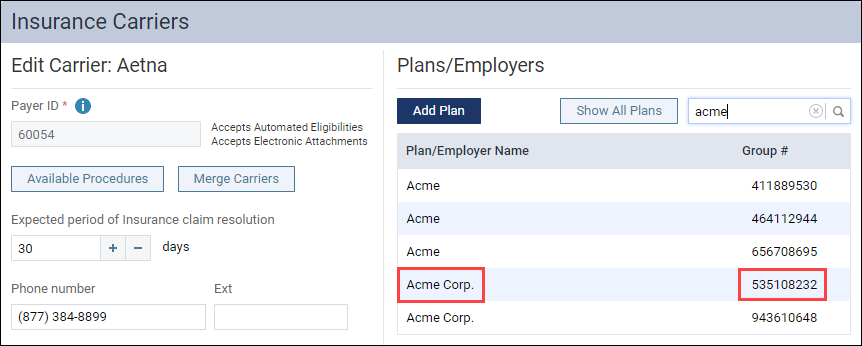
Additional Information
- To learn more about creating insurance plans, watch the Adding an Insurance Plan segment of our webinar 5 Steps to Getting Patient Portion Estimates You Can Trust.
- To learn how to remove duplicate carrier records from your database, watch Merging Insurance Carriers in the Dentrix Ascend Resource Center.
