Do insurance benefits renew automatically? In a word, yes!
Changes to insurance plans usually take place at the end of the plan benefit year. At this time, insurance carriers should provide you with information on what is new and what is changing in your patient’s plan.
In Dentrix Ascend, benefits are reset on the first day of the benefit renewal month automatically. Coverage tables and fee schedules must be manually updated if they change.
If you received advanced notice from the insurance carrier that the benefits will change for the new benefit year, here is the workflow to complete after the benefit renewal. If there are no changes to your patient’s insurance, there is nothing else for you to do.
How to:
Locate the insurance carrier’s new plan via their website or a printed confirmation that your practice received from the insurance carrier. Next, you will update the corresponding insurance plan in Dentrix Ascend.
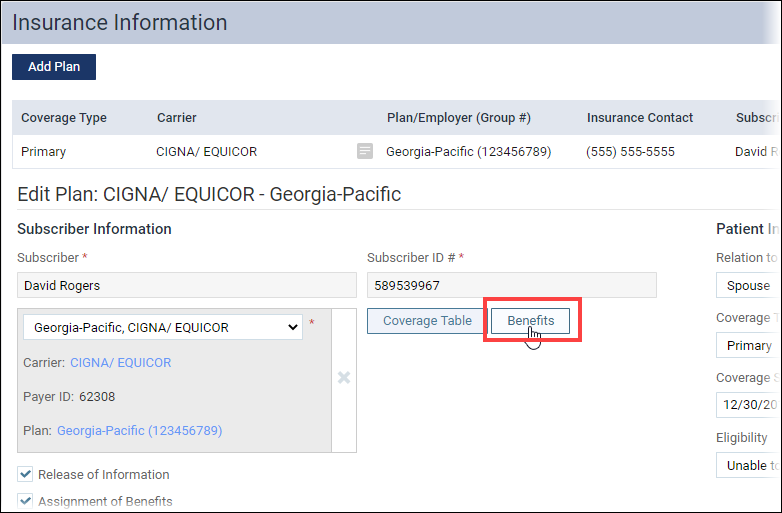
1. Open the Insurance Information page for one of the patients who is on the plan to be changed. Click Benefits to open the insurance carrier’s Deductible and Benefits table.
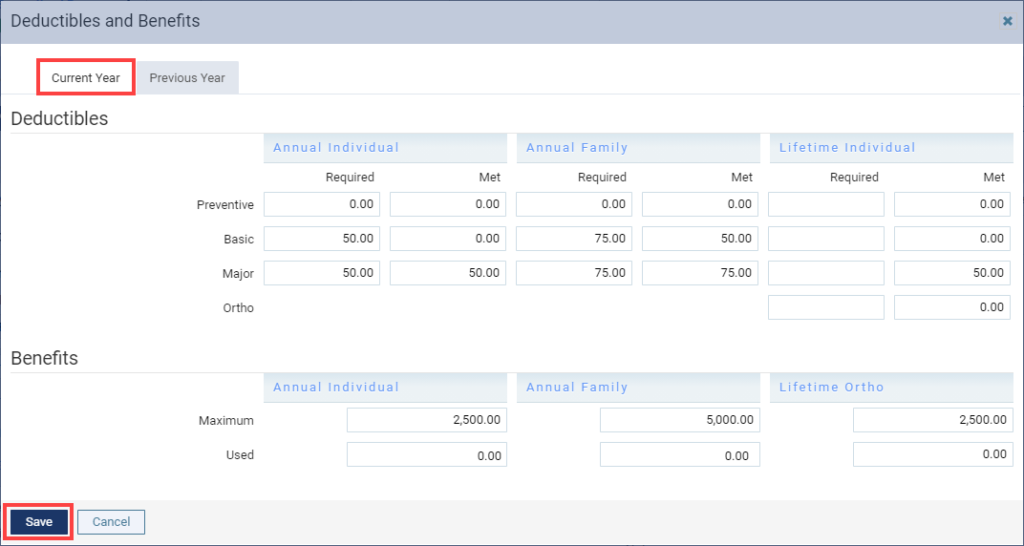
2. Make sure you are looking at the Current Year tab. After referencing the insurance carrier’s plan for the new benefit period, enter the new deductibles and benefits. IMPORTANT: Make these changes AFTER the start of the new benefit period. Note that changing the benefits and deductibles for one patient changes the benefits and deductibles for ALL patients attached to this plan.
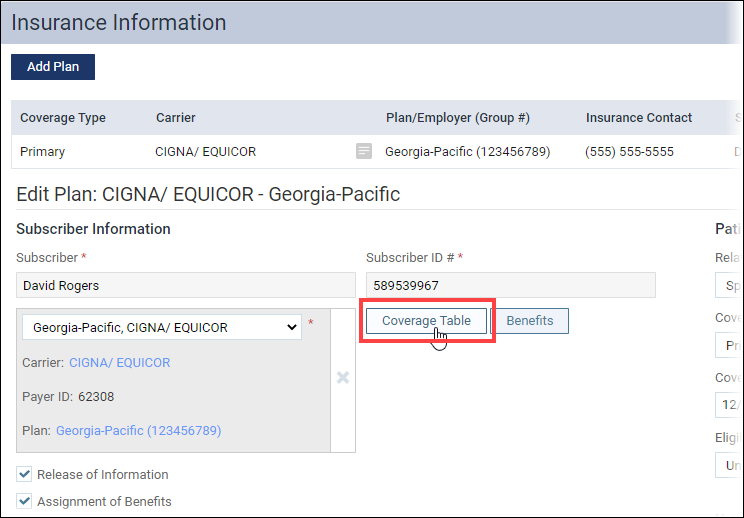
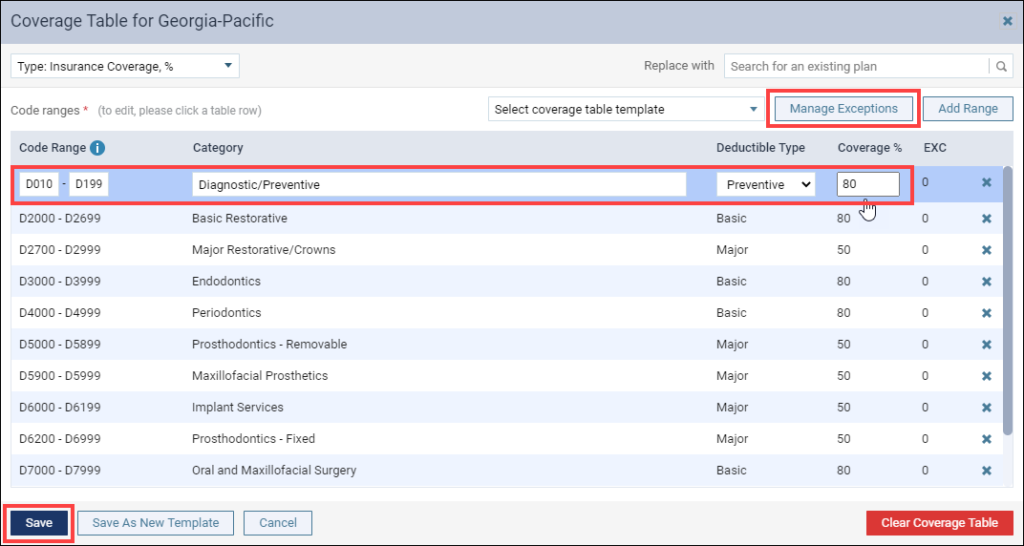
3. Click Coverage Table to open the insurance plan’s coverage table.
4. After referencing the insurance carrier’s plan for the new benefit period, update the coverage table and exceptions.
Additional Information
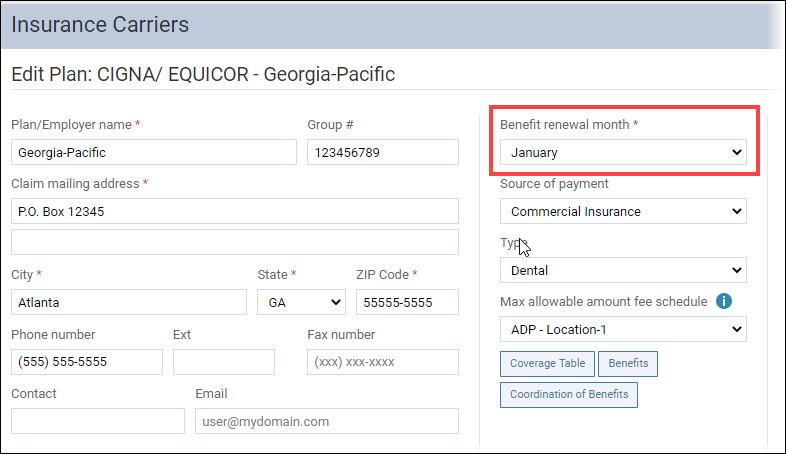
- To learn how to locate an insurance carrier’s benefit renewal month in Dentrix Ascend, read Updating insurance plan information in the Resource Center.
- Fee schedules can be set to expire on a given date and use different values after that date. To learn more, read Updating fee schedules in the Resource Center.
